Blog
25
Apr
Lenacapavir: The Twice-Yearly HIV Prevention Injection Changing Everything
Lenacapavir: The Twice-Yearly
HIV Prevention Injection
Chang...
06
Apr
Generic ED Medicines vs Branded: Why Tariffs Make Generics the Smart Choice in 2026
💊 Breaking News | April 2026
Generic ED Medicines vs Branded:
...
04
Apr
COPD in 2026: Best Inhalers, Medicines & Treatment Guide
Respiratory Health · April 2026
...
01
Apr
Awiqli (Insulin Icodec): The Once-Weekly Insulin Changing Diabetes Forever
Awiqli (Insulin Icodec): The Once-Weekly Insulin Changing Diabetes Forever
Introduction
More t...
29
Mar
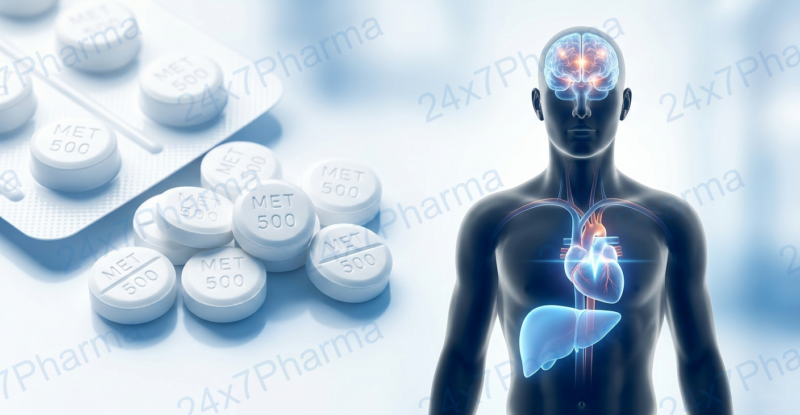
Metformin in 2026: New Uses Beyond Diabetes
Metformin in 2026: New Uses Beyond Diabetes
Introduction
Over 422 million people live with diabetes worldwide, according to the WHO...
28
Mar
Sildenafil vs Tadalafil in 2026: Which ED Pill Is Right for You?
Sildenafil vs Tadalafil in 2026: Which ED Pill Is Right for You?
Erectile dysfunction (ED) affects over 322 million men worldwide, acc...
27
Mar
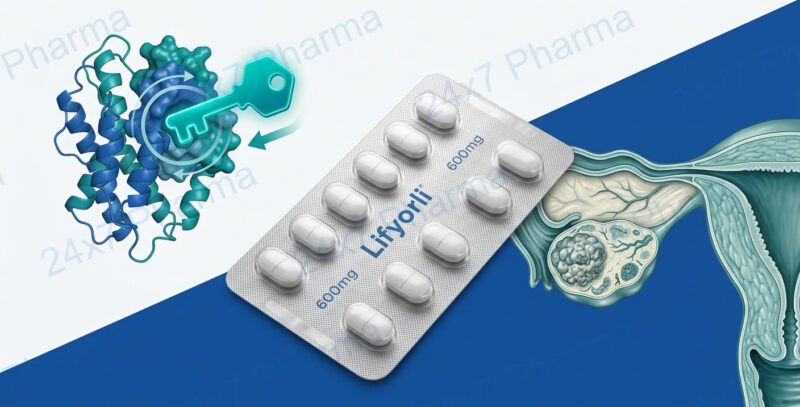
Lifyorli relacorilant for platinum-resistant ovarian cancer
Lifyorli (Relacorilant): The World’s First Cortisol-Blocking Cancer Drug That Makes Chemotherapy Work Better in Ovarian Cancer
I...
26
Mar
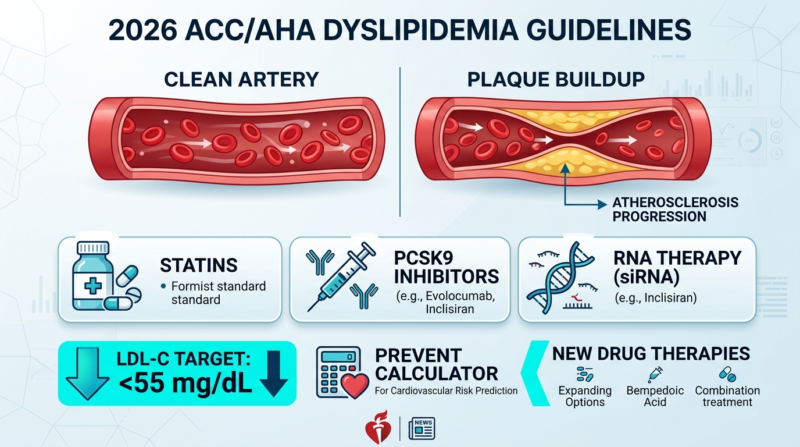
2026 ACC/AHA Dyslipidemia Guidelines: New LDL Targets, PREVENT Calculator & What Changed | 24x7Pharma
2026 ACC/AHA Dyslipidemia Guidelines: Everything Has Changed About How We Treat Cholesterol
A pharmacist-reviewed guide to t...
22
Mar
Oral GLP-1 Pills: Revolutionary Weight Loss Without Injections | 24x7Pharma
Oral GLP-1 Pills (Wegovy Pill & Orforglipron): Revolutionary Weight Loss Without Injections
A complete pharmacist-re...
27
Sep
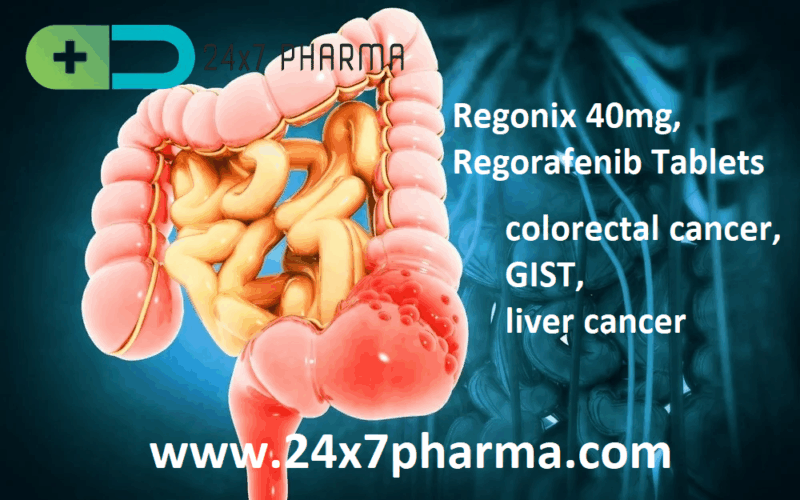
Regonix 40mg: The Power of Multikinase Inhibitors
Regonix 40mg: The Power of Multikinase Inhibitors
Targeted Treatment for Metastatic Colorectal Cancer
Meta Description: Discover ho...
26
Sep
Empowering the Immune System: The Magic of Nivolunix 100mg
Cancer treatment has advanced significantly with the advent of immunotherapy drugs, and among them, Nivolumab has gained wide recogniti...